What Causes Degenerative Disc Disease?

Spinal Degeneration: An Unfortunate Reality of Aging
Consisting of 33 independent bones, your spine acts as the central supporting pillar of your body. These 33 distinct vertebrae link together to create one continuous and cooperative team of bones. With the help of surrounding ligaments and muscles, your spine operates to hold your body upright. Furthermore, your spine enables you to bend, turn, sit, stand, and complete various everyday activities.
When you really stop and think about it, we can almost expect spinal degeneration to occur over time. After all, like a car that wears down after miles of overuse, the spine also begins to break down naturally.
At the best of times, this degeneration can lead to minor aches and pains. While at the worst of times, debilitating discomfort can bring your day to a screeching halt. Although back pain is a reality of life, you may not have realized that your intervertebral discs constitute one of the most vulnerable parts of your spine.
The Details of Disc Degeneration
Degenerative disc disease is an especially common condition among older adults. It primarily affects intervertebral discs, but additional structures, such as the spinal cord, can also be affected, as degenerated discs suffer bulging or herniation.
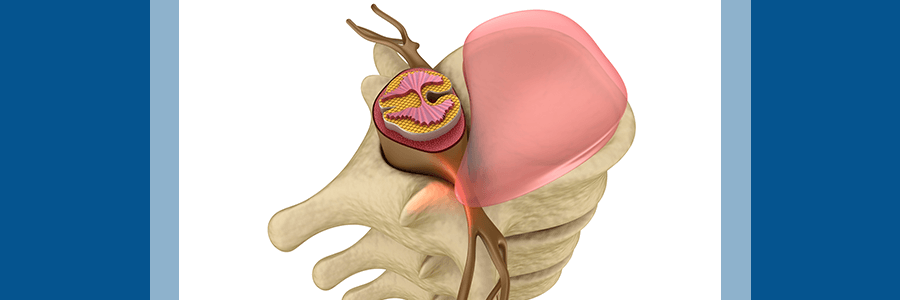
Your intervertebral discs act as cushioning buffers to mitigate the forces between your vertebrae. Like a jelly donut, these discs contain a tough, rubbery outside called the annulus and a jelly-like interior called the nucleus pulposus that provides additional shock absorption to the disc.
When healthy, these discs provide a lubricating barrier between our vertebrae as the spine moves and swivels around. In addition, these discs absorb the impact of bumps and jolts that create pressure on our spine.
However, as time goes by, our intervertebral discs can lose their malleability. Their spongy, resilient characteristics diminish, and the disc itself deflates like an old party balloon. Similar to the deterioration of that old balloon, these aging discs can crumble or even burst open. Often called a slipped or bulging disc, a distended disc can cause pain, tingling, and numbness.
Furthermore, degenerative disc disease can lead to compression of surrounding nerve tissue and a loss of height between our vertebrae. Our bones may begin to rub painfully against one another, accelerating the degradation process. Likewise, bone spurs can develop, leading to even more pinched nerves and restricted spinal mobility.
It’s all just one, slippery slope really. A snowball effect of degeneration. But, if degeneration occurs as a natural part of aging, why do some people experience incapacitating neck and back pain… whereas others beat the odds?
One answer lies in the fact that certain circumstances and conditions can accelerate the progression of degenerative disc disease.
Degenerative Disc Disease Causes & Precipitating Factors
Many risk factors can lead to degenerative disc disease. Four of the most common include:
- Age: As explained above, the aging process can cause the spine to erode, which causes a degenerative cascade of painful symptoms. In fact, most of our body’s tissues tend to dry out, wrinkle, and become more fragile as we age. Think of your skin, hair, nails—and yes—even your eyes, which lose some of their color and vision capacity. The spine is no different.
- Chronic Strain: To be honest, chronic strain from prolonged stress constitutes one of the biggest contributors to degenerative disc disease. This only intensifies when we use improper lifting techniques over a long period of time. Occupations such as nursing, construction, warehouse work, and mechanics can place excessive strain on the back. Lifting heavy objects in awkward positions, whether patients or 2×4’s, can wear on the vertebrae and their connective tissues. A damaged disc can occur over time, or in the blink of an eye.
- Weight: Lifestyle also plays a prominent role in intervertebral disc health. This can be especially true when it comes to weight. Excess body weight in the abdomen and upper body can place unnecessary stress on the spine. Remember: With our every step, the spine absorbs the normal shock from walking and the additional force of our weight.
- Alcohol & Smoking: It’s no surprise that smoking and alcohol aren’t the best choices for you. And, neither are particularly good for the spine. Aside from interrupting normal bone growth, both alcohol and smoking strip our body of vital minerals that keep tissues supple and healthy.
Moreover, degenerative disc disease can also lead to a number of unwanted and painful disorders. These conditions include: spondylolisthesis, facet joint disease, osteoarthritis, spinal stenosis, and herniated discs. Like we said before: It’s all one big, slippery slope.
What Can I Do to Prevent/Treat Degenerative Disc Disease?
The good news, however: We can counteract the development of degenerative disc disease by using a number of easy interventions. Pain management through over-the-counter medications, physical therapy, strength-building in the spine, as well as lifestyle changes can keep the progression at bay. Even a new mattress can help in some situations.
However, when in doubt, consult with your physician or board-certified orthopedic specialist. A spine expert, such as Dr. Frazier, can accurately diagnose your pain and recommend both conservative and minimally invasive solutions.
